Johns Hopkins Experts Use New Tech to Help Distinguish Stroke from Inner Ear Conditions
May 30, 2018
Every year at hospital emergency departments across the country, clinicians evaluate 4.4 million patients whose chief complaint is dizziness or vertigo. About a quarter to a third clearly have a benign inner ear condition (such as benign paroxysmal positional vertigo [BPPV] or vestibular neuritis, a self-limited, inner ear infection/inflammation) that doesn’t require neuroimaging or additional urgent testing. About 5 percent of the time, dizziness is due to a stroke, an emergency situation that necessitates immediate care. Many of the remaining patients have unclear or medical causes for their dizziness—leaving them in an ambiguous gray area for evaluation and treatment (see Figure 1).
For patients presenting with continuous dizziness, nausea/vomiting, and rhythmic involuntary eye movements (called nystagmus), a three-part eye exam was developed by Johns Hopkins neurologist David Newman-Toker, director of the Division of Neuro-Visual and Vestibular Disorders, and colleagues. Known as HINTS (an acronym for Head-Impulse—Nystagmus—Test-of-Skew), the test can detect stroke (as opposed to vestibular neuritis) with high sensitivity and specificity, superior to even magnetic resonance imaging (MRI) acutely. The biggest problem, says Newman-Toker’s neurology colleague Daniel Gold, is that learning how to perform and interpret the test can take months or years of mentorship.

In order to bring this subspecialty expertise to the bedside, Gold and his colleagues are now offering a “Tele-Dizzy” service—a telemedicine approach in which patients who arrive at the Johns Hopkins Hospital emergency department can be evaluated by a technician using portable video-oculography (VOG) goggles with HINTS (and additional tests including Dix-Hallpike positional testing to diagnose BPPV), with Gold and his colleagues interpreting the results remotely. The Tele-Dizzy service is currently offered at just the Johns Hopkins Hospital during weekday business hours, but the team is actively working to expand it to other hospitals throughout the Johns Hopkins system and beyond — at any time of the day or night.
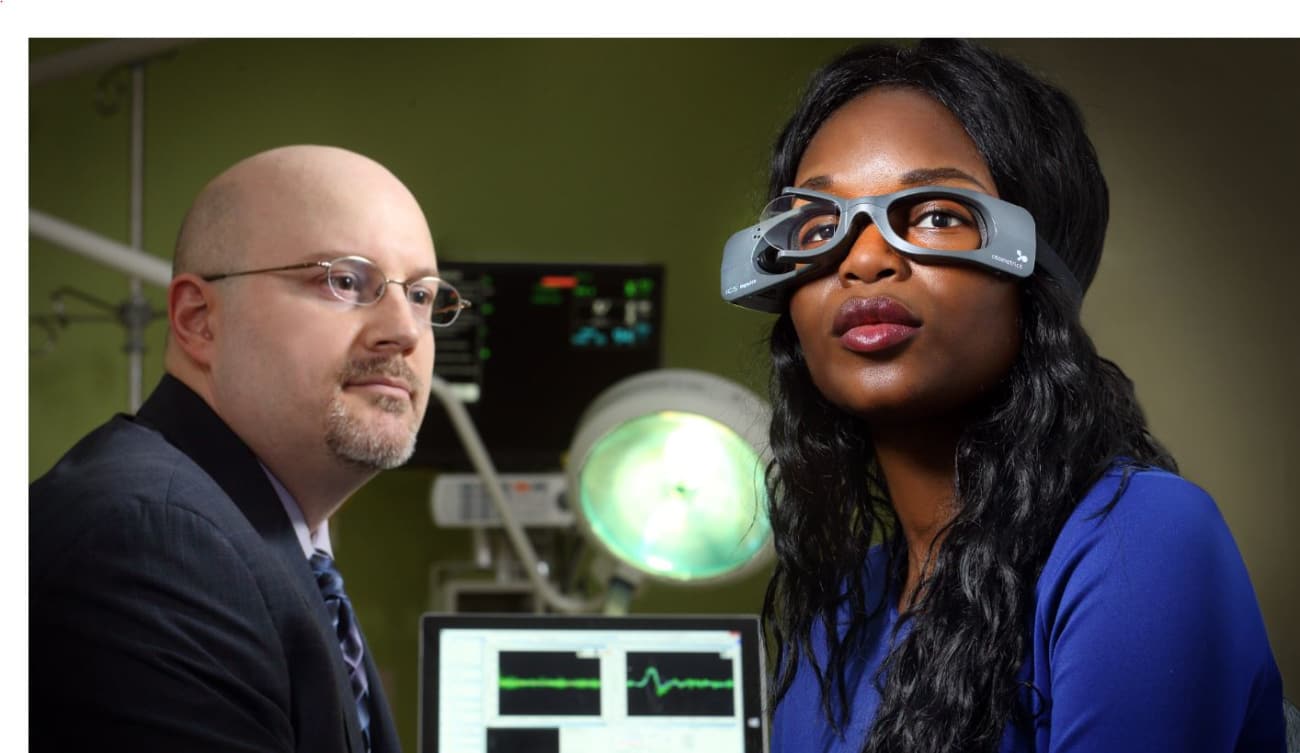
Patients with dizziness or vertigo don VOG goggles that gather tracings of their eye movements while a technician administers the eye movement tests. These eye tracings and videos are then sent to Gold or other experts on call to help diagnose the cause of the dizziness and decide whether a patient is suffering from a benign or dangerous condition (see Figure 2).

“It’s like an electrocardiogram for the eyes,” Gold explains. “Rather than someone with chest pain coming in and getting leads placed on their chest, someone who’s dizzy can come in and put on goggles so we can determine the best next steps.”
The benefits are multifold, Gold adds. Tele-Dizzy has the potential to save time—the testing requires minimal space and the equipment is portable, so in the time that a patient would normally wait for an available room in the ED, testing can be completed and disposition recommendations made. It can also save some of the estimated $1 billion wasted annually in the U.S. on unnecessary MRIs, CT scans, and hospital admissions for patients with non-neurologic causes of dizziness (see Figure 1).